LAST UPDATED: May 1st, 2015
Imagine being told a spirochete has invaded your brain, tissues and organs, causing irreparable damage. Hard to imagine isn’t it? In fact, we tell ourselves, “That kind of thing happens to the other guy.” If you are a hunter, and you don’t take Lyme disease seriously, you may be at risk. Each time you go outdoors in tick-infested territory you run the risk of a tick-borne infection. Specifically, Lyme disease; often called the Great Imitator because it mimics over 300 other diseases.
Ticks are a common (often hazardous) part of the outdoor/bowhunting experience and they can affect you in a number of unwanted ways.
EARLY ONSET
I can’t begin to count the number of ticks we have removed from persons, clothing and gear over the past 30 years of bowhunting, but it is a lot. We have never encountered the tell-tale circular rash around a bite that indicates infection with Lyme disease, but that is not always a guarantee of safety. An estimated 20% of victims may not have the red-ringed rash known as erythema migrans (EM). Caused by an inflammatory response to the infection, a rash may also appear on an area of the body not associated with the tick bite.
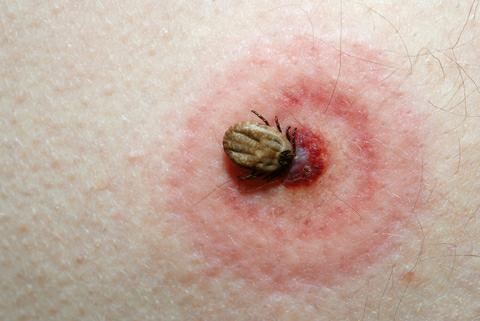
Not all tick bites look like this. In fact, nearly a quarter of tick bite victims have no rash that resembles this.
In speaking with a number of people who were diagnosed with Lyme disease I was surprised to find varied descriptions of symptoms. Although several had similar symptoms, they all described different symptoms. One person had abscessed teeth and gums, while another had terrible knee pain. Early symptoms include fever, fatigue, depression, muscle soreness and headache. These flu-like symptoms may contribute to the initial misdiagnosis. The key to eliminating the localized infection is early diagnosis. With proper antibiotics, the disease can be defeated.
ADVANCED SYMPTOMS
Misdiagnosed Lyme disease is possible as the medical community continues to disagree whether chronic Lyme disease even exists. For those who suffer through months or years of misdiagnosis the consequences can be dangerous. Advanced symptoms may involve the heart, joints and central nervous system. Migrating muscle pain, heart palpitations, dizziness or arthritis-like symptoms may occur. Lyme arthritis can develop, usually affecting the knees. It may also impact ankles, elbows, wrists, hips and shoulders. Pain is often mild or moderate with swelling of the joints.
As symptoms progress they may become disabling, mimicking other diseases like Lupus, Celiac disease, HIV or Lou Gehrig’s disease. One patient I talked to, who had gone misdiagnosed for more than 2 years, was once referred to an infectious disease specialist. The doctor did not believe in chronic Lyme disease. He tested the patient for all of the above diseases. The tests were negative. Still, the doctor wanted to send the patient home with pain killers and medication for depression. Thankfully, the patient consulted other doctors and was finally diagnosed correctly with chronic Lyme disease. He is now undergoing aggressive treatments, but still has an uphill battle to return to normal.
SOURCE OF THE INFECTION
Lyme disease is spread through the bite of a tick infected with a species of bacterium called Borrelia burgdorferi (Bb). It is spiral-shaped, mobile, bacterial organism called a spirochete. It was first discovered on 1975 in the town of Lyme, CT, hence the name. It is the most common tick-borne disease in North America, which means hunters are likely to encounter an infected tick at some time in their life. No proof exists but it is suspected that the bacteria may have been carried to America from Europe during the time of pilgrims, riding the seas on a stowaway rodent.
Spring and summer food plot preparation is a great time and place to encounter a tick.
Commonly called black-legged ticks or deer ticks, these hard bodied ticks of the genus Ixodes are the primary suspects. When the tick is very small, in what is called the nymphal stage, it may have a chance to feed longer, going unnoticed because of its tiny size. We often call them seed ticks. The Center for Disease Control and Prevention (CDC) explains that “Most humans are infected through the bites of immature ticks called nymphs. Nymphs are tiny (less than 2 mm) and difficult to see; they feed during spring and summer months. The tick must be attached for 36-48 hours or more before the Lyme disease bacterium can be transmitted.” Adult ticks may also transmit the bacteria, but are more likely to be discovered and removed due to their larger size. Adult ticks are more active during cooler months. Handling deer, rabbits or squirrels may also bring you in contact with ticks that may spread the disease. Rodents and pets may bring infected ticks into your yard or home, but the American dog tick is not known to transmit the infection.
TREATMENT
According to the CDC, “Patients treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly and completely. Approximately 10-20% of patients (particularly those who were diagnosed later), following appropriate antibiotic treatment, may have persistent or recurrent symptoms and are considered to have Post-treatment Lyme disease syndrome (PTLDS).
While at the SHOT Show I randomly started asking people if they knew someone who had Lyme disease and was shocked to get a “yes” from each person I asked. It is not uncommon for persons afflicted with Lyme disease to see several doctors before being properly diagnosed. Victims stressed seeking out a Lyme-literate doctor. How do you find one? Good question. Most said, “Just start asking questions.” One of the most renowned Lyme-literate doctors is Dr. Joseph G. Jemsek, an Infectious Disease Specialist in Lyme Borreliosis and Tick-Borne infection and HIV/AIDS. He is founder of Jemsek Specialty Clinic of Washington, D.C. Dr. Jemsek prefers the term Lyme Borreliosis Complex (LBC). According to his web site this term, “better reflects an immune-compromising syndrome affecting multiple organ systems and caused by coexisting infections.”
Most often, getting rid of the disease comes down to finding the right physician.
Not only is it bad enough getting Lyme disease, the ticks may carry additional bacteria capable of transmitting additional infections further complicating the diagnosis and treatment. Treatment of advanced cases is much more difficult. There is much dissention in the medical community whether chronic Lyme disease exists. Tests are not always accurate and specific tests need to be done, along with analysis of symptoms, to aid in confirmation of the diagnosis.
PREVENTION
The best way to combat Lyme disease is to prevent the tick bite. Sprays that contain more than 20% DEET may be applied directly to the skin according to product instructions. More effective are products containing permethrin. This is only to be sprayed on clothing and should be allowed to dry prior to wearing. It remains effective with several washings. Pre-treated clothing is also available that is reported to last through 70 washings. Be sure to treat gear, boots, tents etc.
Any time you go afield be mindful of ticks and prepare for them accordingly.
Bathing or showering as soon as possible is important. Conduct a full-body inspection, giving special attention to hair where ticks may be more difficult to locate. Look over your gear and pets each time you have been outdoors. Tumble dry clothes on high heat in the dryer in an effort to kill ticks you may have missed.
Conclusion
A statement on Dr. Jemsek’s web site brings it into perspective, “It is understood de facto that reports of various diseases to the CDC are underreported, but LD may be the all-time winner for underreporting so far as we are concerned. We believe that up to 90% of cases are unrecognized and/or unapparent to the host.”